|
4/3/2024 0 Comments Normal hip joint space xray 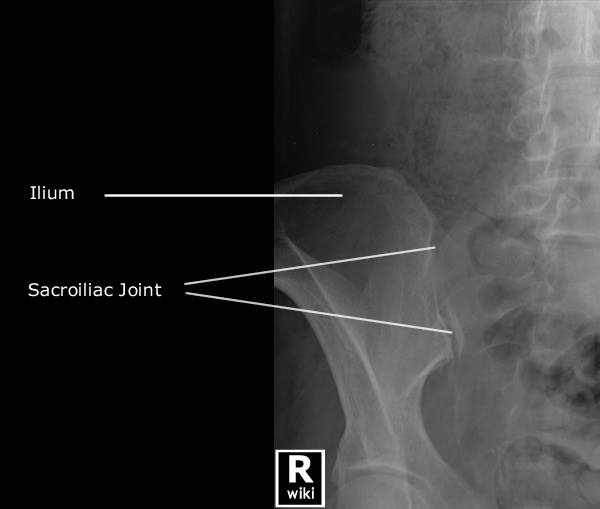
Assessment of knee OA severity relies mainly on JSN and subchondral bone lesions. Once a knee exhibits JSN in either the medial or lateral tibiofemoral compartment, the knee is classified as osteoarthritic despite the absence of obvious osteophytes. Radiographic knee OA is defined as KL grade 2 or above: that is, the presence of a definite marginal osteophyte (KL grade 2), the presence of JSN (KL grade 3), or bone-on-bone contact (KL grade 4). Instead, radiography allows an indirect estimate of cartilage thickness and meniscal integrity by assessment of JSW in the patellofemoral and tibiofemoral joints.Īt present, radiographic diagnosis of knee OA is based on the Kellgren-Lawrence (KL) grading system, a semiquantitative composite score that is based on two radiographic features: the presence of osteophytes and JSN. Radiography can clearly visualize bony features, such as marginal osteophytes, subchondral cysts, and sclerosis, that are characteristic features of OA, but direct visualization of cartilage is not possible. Radiographs are used in clinical practice to establish the diagnosis of OA and to monitor the progression of the disease. We will explain the strengths and limitations of both imaging modalities on the basis of available evidence from the literature and elucidate why today MRI should be considered the imaging modality of choice for cartilage assessment in the context of OA of the knee joint. In this review, we will first describe the current role of conventional radiography for cartilage assessment in OA and then discuss the current and future roles of MRI for the evaluation of cartilage pathology in OA. In contrast, magnetic resonance imaging (MRI) allows direct visualization of cartilage, and technologic advances have led to sophisticated tools such as high-resolution morphologic imaging and compositional or biochemical assessment. Loss of joint space width (JSW), or joint space narrowing (JSN), is considered a surrogate marker for cartilage damage. For decades, direct imaging of cartilage was not possible and investigators relied instead on indirect methods using conventional radiography. Damaged cartilage is one of the key tissues in the disease process that is understood as osteoarthritis (OA), a multi-tissue disease leading eventually to joint failure. Hyaline cartilage is an important intra-articular structure that is prone to damage by trauma or degeneration. Detection of joint space narrowing on radiography seems outdated now that it is possible to directly visualize morphologic and pre-morphologic changes of cartilage by using conventional as well as complex MRI techniques. Moreover, compositional MRI allows imaging of 'pre-morphologic' changes (that is, visualization of subtle intrasubstance matrix changes before any obvious morphologic alterations occur). MRI enables accurate measurement of longitudinal changes in quantitative cartilage morphology in knee osteoarthritis. 'Pre-radiographic' cartilage changes depicted by MRI can be measured reliably by a semiquantitative or quantitative approach. MRI enables visualization not only of cartilage but also of other important features of osteoarthritis simultaneously. With the availability of advanced magnetic resonance imaging (MRI) scanners, new pulse sequences, and imaging techniques, direct visualization of cartilage has become possible. However, radiography is severely limited by its inability to visualize cartilage, the difficulty of ascertaining the optimum and reproducible positioning of the joint in serial assessments, and the difficulty of grading joint space narrowing visually. Loss of joint space width, or 'joint space narrowing', is considered a surrogate marker for cartilage thinning. Imaging of cartilage has traditionally been achieved indirectly with conventional radiography. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
